Eczema concerns?
Get instant expert guidance with our smart AI platform.
Join NowEczema is a common skin condition affecting millions worldwide. It leads to dry, itchy, and inflamed skin, making life uncomfortable for those dealing with it. While more common in children, eczema can occur at any age and is recognized as a systemic inflammatory disease. Though the exact cause isn’t fully understood, both genetic and environmental factors are known to trigger eczema flare ups. In this guide, we’ll explore what eczema is, its causes, and how you can effectively manage its symptoms.
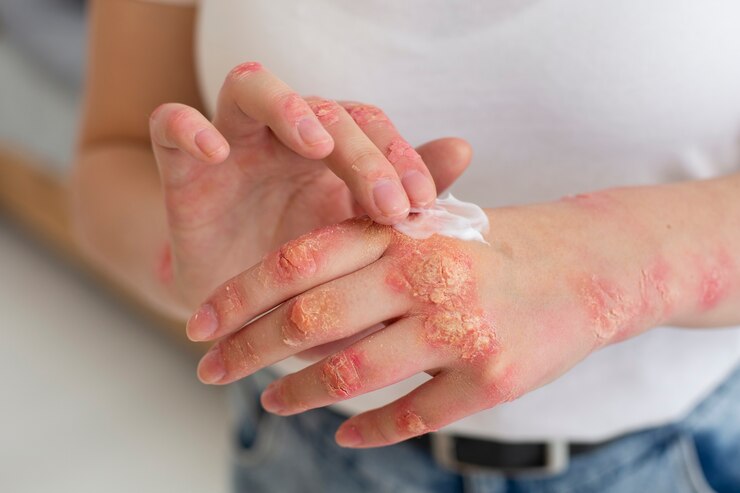
Eczema, also known as atopic dermatitis (AD), is a chronic condition where the skin becomes inflamed, causing dryness, itching, and irritation. It can appear anywhere on the body but is most common on the face, hands, and behind the knees (flexural areas). Eczema varies significantly in severity, with some people experiencing mild symptoms and others dealing with painful, debilitating flare ups that severely impact sleep and daily function.
There are different types of eczema, with atopic dermatitis being the most common. Other forms include contact dermatitis, triggered by irritants or allergens, and dyshidrotic eczema, which causes deep blisters on the hands and feet.
Eczema is often the first manifestation of a condition known as the Atopic March. This describes the natural progression of atopic (allergic) diseases: patients, particularly children, often develop eczema first, followed by food allergies, asthma, and allergic rhinitis (hay fever). This connection underscores that eczema is not just a skin condition, but a systemic immune disorder. Managing eczema aggressively early on may help prevent the progression of other atopic diseases.
The exact cause of eczema is still uncertain, but researchers believe it results from a combination of genetic and environmental factors.
People with a family history of eczema, asthma, or allergies are more likely to develop it. A primary genetic factor is often a malfunction in the skin’s protective barrier, specifically a deficiency in the protein filaggrin. This deficiency leads to moisture loss and easier penetration of irritants.
Additionally, those with eczema may have an overactive immune system, which reacts strongly to otherwise harmless triggers (cytokines like IL 4, IL 13, and IL 31), causing the characteristic redness and intense itching.
External factors that worsen the condition include harsh soaps, certain fabrics (like wool), and dramatic weather changes (cold/dry air or heat/sweat). Allergens, such as pollen and pet dander, along with stress, are also significant contributors to eczema flare ups.
Eczema symptoms vary from person to person but typically include dry, relentlessly itchy skin. The skin may also become red, swollen, or develop cracked patches. In individuals with darker skin tones, the rash may appear gray, brown, or purplish rather than distinctly red.
Symptoms often manifest in a damaging cycle:
Some people experience periods where their symptoms worsen, known as flare ups, followed by times where their skin improves, referred to as remission.
Though there’s no cure for eczema, there are ways to manage it effectively. The primary goal is to minimize flare ups, control inflammation, and aggressively repair the skin barrier. Here’s how:
Moisturize regularly with thick, fragrance-free creams or ointments, especially immediately after bathing (the “soak and seal” method), to lock in moisture and patch the faulty barrier. Look for ingredients like Ceramides and Petrolatum.
For active flare ups, topical treatments like hydrocortisone creams help reduce inflammation. In more severe cases, stronger prescription medications, including Topical Calcineurin Inhibitors (TCI) or JAK/PDE4 inhibitors, may be required as steroid free alternatives.
For moderate to severe cases unresponsive to topicals, systemic therapies are used. These include Biologics (e.g., Dupixent) or oral JAK Inhibitors, which target the underlying immune pathways causing the inflammation.
Wear soft fabrics like cotton, avoid extreme temperatures (heat and sweat are major triggers), and use a humidifier during dry weather (especially winter).
Identify and avoid irritants such as harsh soaps, chemical fragrances, and allergens that might worsen symptoms. A dermatologist can help determine if patch testing is needed.
Natural remedies like colloidal oatmeal baths and virgin coconut oil can soothe the skin, though it’s best to consult with a healthcare provider before trying new treatments.
By combining these strategies and staying mindful of your triggers, eczema symptoms can be managed effectively, leading to clearer skin and improving your quality of life.
Like many of you, our eczema journey is personal. That’s why we’re committed to creating a space for the eczema community to share experiences, be empowered through evidence-based solutions, and learn practical tips for daily life.
– Sajjad, Founder & CEO of NellaDerm
