Eczema concerns?
Get instant expert guidance with our smart AI platform.
Join NowStaphylococcus aureus (staph) loves broken or very dry skin. During eczema flares, tiny cracks and constant scratching make it easier for staph to settle on the surface, irritate skin, and sometimes cause infection. The goal is not to sterilize your skin; it is to lower staph load, protect the barrier, and recognize early signs of trouble. This guide translates dermatology advice into daily steps you can actually follow so staph eczema stops hijacking your week.
A large systematic review from British Journal of Dermatology found that people with atopic dermatitis carry S. aureus on their skin and in the nose far more often than people without eczema, helping explain why “staph eczema” is so common during flares.
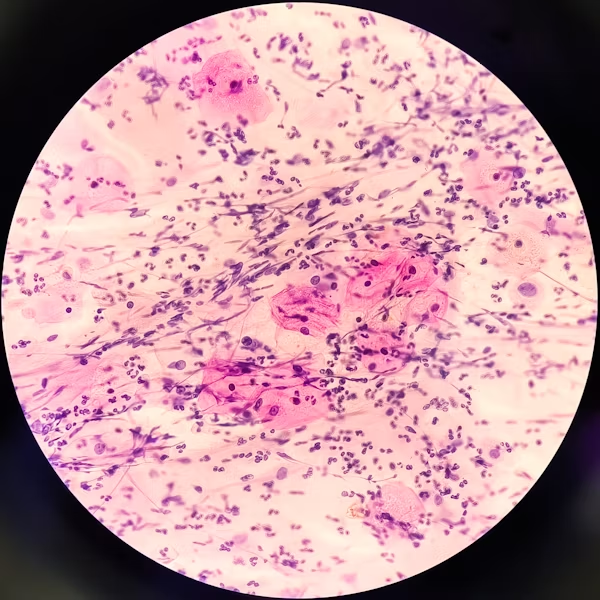
If any of these show up, seek medical care promptly.
Always follow your clinician’s plan. The ideas below are common tools. Your provider will tell you which fit your skin, history, and age.
If you are curious why clinicians emphasize reducing staph burden, the 2016 meta-analysis mentioned previously quantified how common S. aureus carriage is in eczema, helping justify these steps during high-risk periods.
If a patch looks angry but not infected:
If you see yellow crust, increasing pain, or spreading redness: keep the area clean and covered in soft fabric, do not pick or scrub, and seek care the same day.
For step-by-step textile care that helps calm staph eczema, use the laundry guide on NellaDerm.
Children scratch in their sleep and during play, so small habits matter:
Call your pediatric clinician if a child shows spreading redness, fever, oozing, or if itch disrupts sleep several nights in a row.
For a full packing list and rapid-flare sink plan, see the travel essentials article on NellaDerm.
Bring a list of products you use and a simple timeline of the flare; photos from the first day help clinicians judge progress.
You cannot and should not try to scrub skin sterile. The winning strategy for staph eczema is to strengthen the barrier, lower staph load safely, and act quickly if infection appears. Keep cleansing brief and lukewarm, moisturize within three minutes after every rinse, reduce friction and scratching, and follow your clinician’s plan for antiseptic or decolonization steps when needed. If warning signs show up, seek care promptly. Early treatment plus steady daily habits keep infections from dictating your life.
Is “staph eczema” contagious?
Eczema itself is not contagious. Staph bacteria can pass between people through skin-to-skin contact or shared items, but good hygiene and intact skin make this much less likely.
Should I swab my skin for staph?
Swabs are sometimes used when infections are recurrent or severe. Most day-to-day eczema care does not require cultures unless your clinician is concerned about resistant bacteria.
Do bleach baths cure eczema?
No. They can lower surface bacteria and may reduce infection risk for some, but they work with barrier care and your prescribed medications—not instead of them.
Do probiotics or “good bacteria” creams fix staph?
Research on skin probiotics is promising but still developing. Ask your clinician before adding new products; do not skip proven basics while you experiment.
I keep getting painful cracks on fingers or ankles?
Cracks invite bacteria. Increase moisturizer frequency, use cotton liners under gloves for wet work, and cover fissures with soft fabric after sealing them. Seek care if cracks look infected.
It’s easy to apply and isn’t chalky at all. I’ve been applying it multiple times a day… I’ve tried multiple new products to try and treat my eye eczema, and this is definitely the best I’ve tried so far.
My 7-year old son has been dealing with eczema on his face for a long time, and it’s been so tough to find something that really works…..I’m amazed by the results! Within one day, the redness and rough patches on his face significantly improved…. he doesn’t mind using it at all because it doesn’t sting or feel greasy. – Lily




Like many of you, our eczema journey is personal. That’s why we’re committed to creating a space for the eczema community to share experiences, be empowered through evidence-based solutions, and learn practical tips for daily life.
– Sajjad, Founder & CEO of NellaDerm
