Eczema Concerns? Get Answers
Our AI-powered platform provides personalized guidance and relief strategies for your eczema symptoms.
If you’ve used topical corticosteroids to manage eczema for a long time and noticed your skin worsening when stopping them, you’re not alone. You may be experiencing Topical Steroid Withdrawal, commonly referred to as TSW for eczema. This increasingly recognized phenomenon involves a rebound effect where the skin becomes inflamed, painful, and highly reactive after discontinuing steroid creams. But how long does TSW for eczema actually last and what can you expect during recovery?
In this comprehensive guide, we’ll walk through what TSW for eczema is, how to recognize it, the stages of healing, and realistic timelines supported by patient experience and emerging clinical evidence.
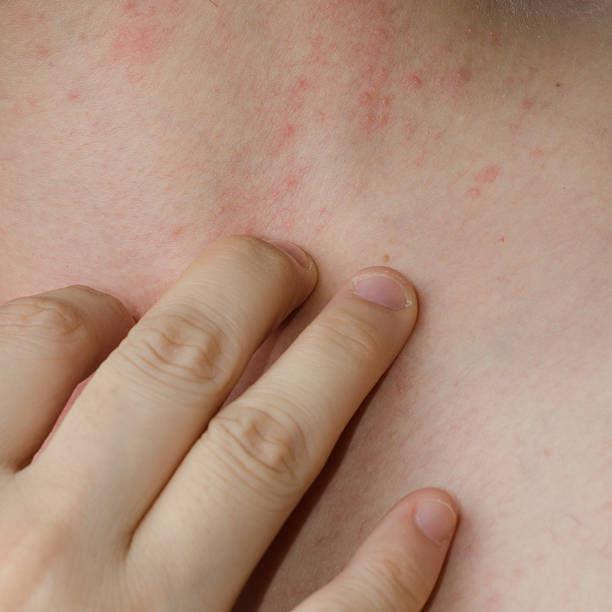
Topical steroid withdrawal, commonly known as TSW for eczema, is a challenging and often misunderstood condition that occurs when the skin reacts adversely after prolonged use of corticosteroid creams. While these medications are highly effective for managing eczema flares, stopping them abruptly or after extended periods can trigger a cascade of intense symptoms that go beyond typical eczema behavior.
For many patients, TSW represents a painful and confusing phase in their eczema journey. Symptoms can be more severe and widespread than standard flares, affecting quality of life, sleep, and mental health. Understanding TSW is crucial for anyone considering reducing or discontinuing topical steroids under medical guidance.
This comprehensive guide explores what TSW is, how it differs from regular eczema, the stages of recovery, and evidence-based strategies for navigating this difficult process safely.
TSW for eczema occurs when the skin becomes dependent on topical corticosteroids. When the medication is stopped, especially after long-term or high-potency use, your skin may enter a state of dysregulation. Instead of returning to its baseline, the skin exhibits symptoms such as burning, flaking, swelling, oozing, and intense itch.
This condition is also called Red Skin Syndrome (RSS). It’s different from a typical eczema flare. TSW often affects larger surface areas, can present symmetrically, and typically includes symptoms not seen in routine eczema, like nerve pain or excessive shedding.
The National Eczema Association acknowledges that while more research is needed, TSW is a real and debilitating condition for many people, often misdiagnosed or overlooked by professionals unfamiliar with the syndrome.
These symptoms can persist for weeks or even years in severe cases, depending on several individual factors.
There is no single answer. Recovery timelines vary widely depending on:
Typical timeframes reported include:
A 2020 systematic review in JAAD International highlights that long-term corticosteroid users (especially over 12 months) are more likely to experience prolonged withdrawal symptoms.
Some people experience “waves” or flare cycles, where they feel healed for a time before symptoms recur. These flare cycles typically reduce in intensity and frequency over time.
It’s important to differentiate between a regular eczema flare-up and TSW:
| Feature | Eczema Flare | TSW for Eczema |
| Itching | ✓ | ✓✓✓ |
| Burning | ✗ | ✓✓✓ |
| Symmetry | Variable | Often bilateral |
| Oozing/Weeping | Sometimes | Often excessive |
| Triggered by steroids | ✗ | ✓ |
| Recovery after stopping steroids | ✓ | ✗ |
Not everyone who uses topical steroids will experience TSW, but certain patterns significantly increase the likelihood. Long-term users, particularly those applying potent or super-potent corticosteroids daily for months or years, face the highest risk. Facial and genital application is especially problematic due to thinner skin and higher absorption rates.
Children and infants are particularly vulnerable because their skin barrier is still developing and they have a higher body surface area to weight ratio, leading to greater systemic absorption. Adults with a history of frequent, high-dose steroid cycles for severe eczema are also prime candidates.
Individuals who “rebound” quickly after short breaks in treatment often show early signs of dependency. Those using steroids under occlusion (like wet wraps) or combining multiple potency levels without medical oversight dramatically heighten their risk profile.
Genetic factors may play a role too. People with filaggrin gene mutations, already prone to severe eczema, might experience more intense withdrawal due to underlying barrier dysfunction. Awareness of these risk factors allows for proactive monitoring and safer steroid management strategies.
Abrupt cessation is the leading trigger for severe TSW. Dermatologists recommend gradual tapering under professional supervision to allow the skin’s natural cortisol production and barrier function to recalibrate. A typical protocol involves reducing potency first, then frequency, over weeks to months.
Start by switching from high-potency to mid or low-potency steroids while maintaining daily application. Once stable, begin interval dosing: every other day, then twice weekly, then once weekly. Monitor skin response at each step and extend intervals if rebound occurs.
Non-steroidal alternatives like calcineurin inhibitors (tacrolimus, pimecrolimus) or PDE4 inhibitors (crisaborole) can bridge the gap during tapering. Emollients applied liberally multiple times daily support barrier repair and reduce the urge to resume steroids during mild flares.
Keep a detailed symptom journal throughout the process. Track application sites, potency, frequency, and skin response. This data helps your dermatologist adjust the plan and distinguish between expected adjustment periods and true TSW onset.
While TSW requires time to resolve, several supportive measures can ease discomfort and promote healing. Cool compresses applied for 10 to 15 minutes several times daily provide immediate relief from burning and inflammation. Use clean, soft cloths soaked in cool water or chilled physiological saline.
Bathing routines should be gentle and brief. Lukewarm water for five to ten minutes with fragrance-free emollients added directly to the bath helps soothe without stripping natural oils. Pat dry gently and apply thick layers of occlusive ointments immediately to lock in moisture.
Natural anti-inflammatory agents like colloidal oatmeal baths or zinc oxide pastes offer safe soothing properties. Some patients find relief with ice pack therapy wrapped in cloth to avoid direct cold injury. Light cotton clothing and bedding minimize friction and temperature fluctuations.
Sleep disruption is common, so establish a calming bedtime routine. Dim lights, cool room temperature, and white noise can improve rest. Over-the-counter antihistamines may help with itching at night, but consult your doctor first to avoid interactions or rebound effects.
TSW affects more than skin. The chronic pain, visible symptoms, and prolonged recovery often lead to anxiety, depression, and social isolation. Many patients describe feeling hopeless during intense flare cycles, especially when progress seems nonexistent.
Online communities dedicated to TSW provide invaluable peer support. Platforms like the ITSAN (International Topical Steroid Awareness Network) forums connect thousands of individuals sharing similar experiences. Reading recovery stories from those further along the timeline offers realistic hope and practical tips.
Professional mental health support is equally important. Cognitive behavioral therapy helps reframe negative thought patterns about healing. Support groups facilitated by psychologists familiar with chronic skin conditions create safe spaces to process grief and frustration.
Family education is crucial. Loved ones often struggle to understand the severity and duration of TSW. Sharing reputable resources and inviting them to medical appointments fosters empathy and reduces feelings of loneliness during the recovery journey.
Most TSW cases resolve with time and supportive care, but severe instances may require medical escalation. Dupilumab, a biologic injection approved for moderate to severe eczema, has shown promise in accelerating TSW recovery by modulating the immune response without steroid dependency.
Oral cyclosporine or methotrexate provides short-term immunosuppression for debilitating symptoms, allowing the skin to stabilize before tapering these medications carefully. Phototherapy under dermatologist supervision can reduce inflammation in widespread cases.
Pain management specialists may prescribe gabapentin or pregabalin for neuropathic burning sensations. Low-dose naltrexone is an emerging off-label option showing anecdotal success in reducing nerve pain and inflammation during withdrawal.
Any intervention must be weighed against risks and monitored closely. The goal remains supporting the body’s natural healing rather than suppressing symptoms indefinitely, which could perpetuate the cycle.
The best approach to TSW is prevention through responsible steroid use. Follow the “fingertip unit” rule: one fingertip of cream covers two adult hand areas. Apply only to active lesions, not prophylactically on clear skin.
Limit potent steroids to short bursts of seven to fourteen days maximum. Use mild potency for face, genitals, and skin folds. Implement “steroid holidays” with proactive non-steroidal management using emollients, wet wraps, and trigger avoidance.
Regular dermatologist check-ins ensure objective assessment of treatment necessity. Explore steroid-sparing options early: proactive tacrolimus, crisaborole, or JAK inhibitors for frequent relapsers. Build a robust daily skincare routine with barrier-supporting ceramides and humectants.
Patient education empowers safer choices. Understanding potency classes, absorption differences, and early dependency signs allows collaboration with healthcare providers to minimize long-term risks while controlling eczema effectively.
The silver lining of TSW recovery is often dramatically improved skin resilience. Many patients report their eczema becomes more manageable post-withdrawal, with fewer and milder flares requiring minimal intervention.
Skin tolerance to products increases significantly. Previously reactive individuals find they can use gentle cleansers, moisturizers, and even mild actives without irritation. The skin barrier, once rebuilt naturally, functions more efficiently at retaining moisture and defending against irritants.
Some experience complete resolution of their original eczema, suggesting steroid dependency masked the true underlying condition severity. Others maintain mild eczema but with greater control through lifestyle and non-steroidal management.
Quality of life improvements extend beyond skin. Better sleep, reduced anxiety about flares, and confidence in natural healing processes transform the eczema experience from constant battle to occasional maintenance.
Research into TSW has accelerated in recent years, moving from anecdotal reports to systematic analysis. The 2023 consensus statement from the International Society of Atopic Dermatitis established diagnostic criteria, improving recognition and study consistency.
Biomarker studies explore nitric oxide levels, cortisol suppression, and gene expression changes during withdrawal. These may eventually enable predictive testing for TSW susceptibility before long-term steroid initiation.
Clinical trials investigating dupilumab, JAK inhibitors, and microbiome modulation during TSW aim to shorten recovery timelines. Long-term cohort studies track post-TSW patients to quantify sustained benefits and optimal management protocols.
As evidence grows, medical education curricula increasingly include TSW training. This shift promises earlier recognition, safer prescribing practices, and more compassionate care for those navigating steroid withdrawal.
The terms are related but distinct. Steroid addiction implies psychological dependence, while TSW refers to physiological skin changes after cessation. Many experience TSW without addictive behavior.
Yes, though less common. Prolonged daily use, especially on thin skin areas, can lead to dependency and withdrawal symptoms upon stopping.
No treatment “cures” TSW, but consistent emollient use is foundational for symptom management and barrier repair throughout recovery.
Absolutely not. TSW is a physiological response to medication withdrawal, not an infection or transmissible condition.
While no specific diet cures TSW, anti-inflammatory foods rich in omega-3s, antioxidants, and probiotics support overall healing and may reduce flare intensity.
For gentle, steroid-free eczema management post-TSW, explore NellaDerm’s dermatologist-formulated collection, designed to soothe and strengthen sensitive skin naturally.
Managing TSW for eczema is about patience, barrier repair, and avoiding triggers, not curing the skin overnight. Here’s how to get through it:
Opt for products that soothe without causing irritation. Look for ceramide-rich creams or balms like NellaDerm’s NellaCalm cream, which is formulated without steroids or fragrance.
Some patients find relief by not moisturizing for a period to allow the skin to self-regulate (known as the “no moisture” method). Others do better with consistent, heavy emollients. It depends on your skin’s tolerance.
Use lukewarm water and moisturize within 3 minutes of patting dry. Learn more in NellaDerm’s blog post “How to Use the 3-Minute Rule for Eczema”.
Support the skin’s flora by avoiding antibacterial soaps. Gentle cleansing once daily is usually sufficient.
Track your symptoms, food intake, stress levels, and product use. Patterns will emerge that can help you and your healthcare provider adjust your plan.
Not all dermatologists are familiar with TSW for eczema, so it’s crucial to find one who is open-minded and knowledgeable. Organizations like ITSAN (International Topical Steroid Awareness Network) provide directories and resources.
TSW for eczema can take a severe toll on mental health, especially due to its chronic nature and visible symptoms. Support groups, therapy, and mindfulness practices (such as meditation or journaling) can be invaluable.
TSW for eczema is a tough, often misunderstood journey, but one that thousands of people are navigating successfully. While the process can be long, many who go through it report clearer, calmer skin at the end of the tunnel.
Remember, this journey is not linear. Some days will feel worse than others. But with the right support system, safe products, and skin barrier strategies, recovery is possible.
Explore gentle, non-steroidal skincare products at NellaDerm.com to support your healing journey today.
Q: Can I taper off steroids instead of quitting cold turkey?
A: Yes. In many cases, tapering can reduce the shock to your system. However, TSW may still occur if the skin is already dependent.
Q: Is TSW permanent?
A: No, TSW for eczema is not permanent, but it can take a long time to resolve. Full recovery can take months to years depending on severity and history.
Q: Are biologics like Dupixent a good alternative?
A: Some patients find relief with biologics, but they may not eliminate the symptoms of TSW if dependence has already developed.
Q: Should I use natural remedies during TSW?
A: Be cautious. Even natural ingredients like essential oils can be irritating. Always patch test and consult your doctor.
Our AI-powered platform provides personalized guidance and relief strategies for your eczema symptoms.
It’s easy to apply and isn’t chalky at all. I’ve been applying it multiple times a day… I’ve tried multiple new products to try and treat my eye eczema, and this is definitely the best I’ve tried so far.
My 7-year old son has been dealing with eczema on his face for a long time, and it’s been so tough to find something that really works…..I’m amazed by the results! Within one day, the redness and rough patches on his face significantly improved…. he doesn’t mind using it at all because it doesn’t sting or feel greasy. – Lily




Get expert advice, exclusive offers, and real stories from people who understand your journey.
Start your skincare journey with an exclusive discount
Practical advice for managing sensitive and eczema-prone skin
Be the first to try our latest technology and product releases
Get 10% off your first order when you sign up
Secure & Private
Instant Access
Premium Content
Like many of you, our eczema journey is personal. That’s why we’re committed to creating a space for the eczema community to share experiences, be empowered through evidence-based solutions, and learn practical tips for daily life.
– Sajjad, Founder & CEO of NellaDerm
