Eczema concerns?
Get instant expert guidance with our smart AI platform.
Join NowIf you’ve used topical steroids for eczema and started noticing worsening symptoms, burning skin, or redness that spreads beyond the original eczema site, you may have heard of TSW for eczema, short for topical steroid withdrawal. This controversial and often misunderstood condition is gaining attention among patients and dermatologists alike.
While topical corticosteroids are a mainstay of eczema treatment, overuse or sudden discontinuation can lead to steroid-induced dermatitis or withdrawal reactions. In this post, we’ll explain what TSW for eczema looks like, why it happens, and how to support your skin through the process.
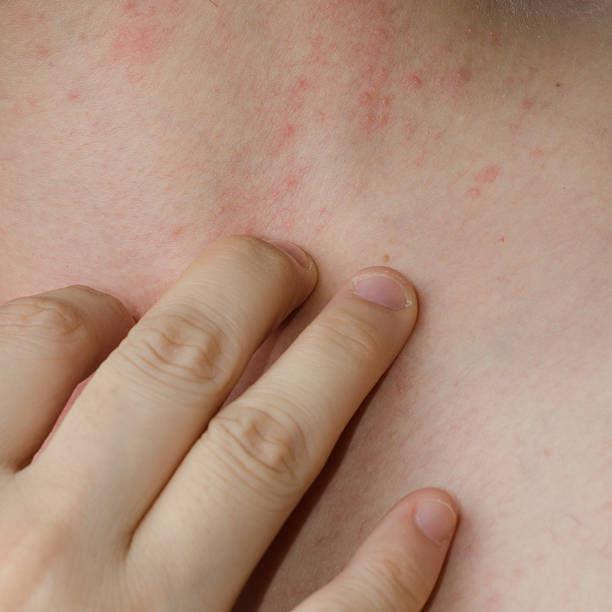
TSW for eczema refers to the withdrawal reaction some people experience after stopping prolonged or high potency topical steroid use. This reaction is not the same as a typical eczema flare it may be more widespread, more painful, and often accompanied by red, burning, and oozing skin, especially on the face, neck, and genitals.
TSW is also known as:
According to a 2023 review in NIH, TSW is often underrecognized and underdiagnosed, but can present after long term steroid use, especially in adults using medium to high potency corticosteroids daily for more than a few weeks.
Topical corticosteroids suppress inflammation by interacting with the immune system. Over time, this can disrupt the skin’s natural healing response, suppress local immunity, and thin the skin barrier.
When steroids are stopped suddenly, especially after chronic use, the skin can rebound which results in widespread inflammation, intense redness, and hypersensitivity to even mild triggers.
People most at risk for TSW include:
Symptoms of TSW for eczema often go beyond a regular flare. Common signs include:
Some patients also report systemic symptoms like chills, fatigue, or swollen lymph nodes.
The course of TSW varies from person to person. For some, symptoms may improve within a few months. For others, especially those who have used steroids for years, withdrawal can last 6 to 24 months or longer.
The ITSAN (International Topical Steroid Awareness Network) estimates that most people improve by 18 to 24 months if they stay completely off steroids. However, recovery can involve cycles of flares and remissions.
The recovery journey from topical steroid withdrawal typically progresses through several distinct phases. Understanding these stages can help patients manage expectations and recognize progress even when symptoms feel overwhelming.
This phase begins within days to weeks after discontinuing steroid use. The skin experiences a dramatic rebound effect with intense redness, burning, and swelling. Many patients describe this as the most challenging period, often lasting several weeks to months depending on previous steroid use duration and potency.
As recovery progresses, the constant severe symptoms begin to break into cycles of flares and remissions. Flares become less frequent and less intense over time, while remission periods grow longer. This pattern indicates the nervous system and skin barrier are gradually recalibrating.
In the final phase, the skin achieves a new baseline. While some sensitivity may persist, the dramatic flares and systemic symptoms subside. The skin barrier function improves significantly, and patients can often reintroduce gentle skincare products without triggering reactions.
There is no universal treatment protocol for TSW for eczema, but supportive care is essential. Below are approaches that many patients and doctors use to support healing:
Some patients find relief with “no moisture therapy,” which reduces moisturizer use to encourage the skin’s own repair mechanisms. Others prefer barrier support with thick, fragrance free emollients.
Try a mid ground approach by applying a gentle, steroid free moisturizer like NellaDerm’s NellaCalm cream, which uses botanical oils and ceramides to soothe inflamed skin.
Cool compresses and wet wraps can reduce burning and hydrate the skin. Some people benefit from oatmeal or vinegar soaks, but always patch test first.
TSW takes a toll on mental health. Mood swings, isolation, and body image issues are common. Mindfulness practices, therapy, and online support groups like ITSAN can provide emotional resilience.
For more on mind body care, see our post on Eczema and Stress Management, where we discuss grounding techniques that can ease both anxiety and inflammation.
While not a cure, some patients report improvements from anti inflammatory diets rich in omega 3s, zinc, and probiotics. Always consult a physician before beginning new supplements or diets.
For those seeking to avoid or reduce steroid use while managing eczema symptoms, several evidence based alternatives exist. These options can help control inflammation without the risk of withdrawal symptoms associated with long term steroid use.
Prescription medications like tacrolimus and pimecrolimus work by suppressing specific immune responses without thinning the skin. These are particularly useful for sensitive areas like the face and neck where steroids should be used cautiously.
Advanced formulations containing ceramides, cholesterol, and fatty acids in the correct ratios can significantly improve skin barrier function. Regular use of these creams may reduce the need for anti inflammatory medications over time.
Controlled exposure to narrowband UVB light under medical supervision can reduce inflammation and itching. Phototherapy offers a systemic approach without the risks associated with topical medications.
For severe cases, newer biologic medications and oral immunosuppressants target specific inflammatory pathways. These require careful monitoring but can provide relief for patients who cannot use topical treatments.
If you’re considering stopping topical steroids, it’s important to talk to a dermatologist familiar with TSW for eczema. Suddenly quitting may worsen symptoms in some cases, while a gradual taper might reduce shock to the system.
Some dermatologists deny the legitimacy of TSW, while others acknowledge it as a subset of eczema patients. Be sure to find a healthcare provider who listens to your symptoms and has experience treating withdrawal.
Prevention remains the best approach to avoiding topical steroid withdrawal. Understanding proper steroid use can help patients benefit from these medications while minimizing risks.
One finger tip unit (the amount of cream that extends from the tip to the first crease of the index finger) covers an area roughly the size of two adult palms. This measurement helps prevent overuse.
After two weeks of continuous use, consider taking a break of equal length while maintaining skin care with non steroid moisturizers and barrier repair creams.
Start with low potency steroids for mild flares and reserve higher potency options for severe, resistant areas. Avoid using high potency steroids on thin skin areas like the face, neck, and groin.
Steroids work best as part of a complete eczema management plan that includes gentle cleansing, regular moisturizing, trigger avoidance, and lifestyle modifications to reduce inflammation.
The topic of TSW for eczema remains controversial. While many patient groups advocate for recognition, mainstream dermatology still debates the condition’s prevalence.
One study observed over 100 patients with suspected steroid addiction and described a clear clinical pattern of worsening symptoms upon withdrawal. More recent literature continues to explore the role of skin barrier dysfunction and steroid dependency.
Navigating topical steroid withdrawal requires more than medical treatment. Emotional support and practical assistance can significantly impact recovery outcomes and quality of life during this challenging journey.
Seek dermatologists who acknowledge TSW as a valid condition or at least approach your symptoms with an open mind. Consider traveling to specialized centers if local options are limited.
Organizations like ITSAN provide educational materials and connect patients worldwide. Social media groups offer real time support but should be balanced with professional medical advice.
During severe flares, simple tasks become challenging. Enlist help with household chores, meal preparation, and childcare. Consider disability accommodations at work or school during the most difficult periods.
Therapists familiar with chronic illness can provide coping strategies for anxiety, depression, and body image issues that often accompany TSW. Some specialize in cognitive behavioral techniques for chronic pain and itching.
TSW for eczema is a difficult but very real journey for thousands of people trying to reclaim their skin health after long term steroid use. While there’s no quick fix, understanding the symptoms and focusing on barrier support, nutrition, and emotional resilience can help the healing process.
If you’re looking for a gentle, steroid free cream that supports recovery, NellaDerm’s NellaCalm cream may be a good option to add to your routine.
For those navigating long term treatment and eczema triggers, our blog on Can You Prevent Eczema in Babies explores early care and long term outcomes for eczema prone individuals.
TSW for eczema may not be easy but with time, support, and the right products, healing is possible.
It’s easy to apply and isn’t chalky at all. I’ve been applying it multiple times a day… I’ve tried multiple new products to try and treat my eye eczema, and this is definitely the best I’ve tried so far.
My 7-year old son has been dealing with eczema on his face for a long time, and it’s been so tough to find something that really works…..I’m amazed by the results! Within one day, the redness and rough patches on his face significantly improved…. he doesn’t mind using it at all because it doesn’t sting or feel greasy. – Lily




Like many of you, our eczema journey is personal. That’s why we’re committed to creating a space for the eczema community to share experiences, be empowered through evidence-based solutions, and learn practical tips for daily life.
– Sajjad, Founder & CEO of NellaDerm
