Eczema concerns?
Get instant expert guidance with our smart AI platform.
Join NowIf you’ve ever asked, “what does eczema look like?”, you’re not alone. Eczema, also known as atopic dermatitis, is highly variable in appearance. Skin presentation can differ by type of eczema, location on the body, chronicity, and even skin tone. Recognizing how eczema looks across different forms is crucial for early identification and effective care.
In this comprehensive guide, we describe the most common eczema types, provide visual cues for different stages and tones, offer expert skincare tips, and help you know when to seek medical input.
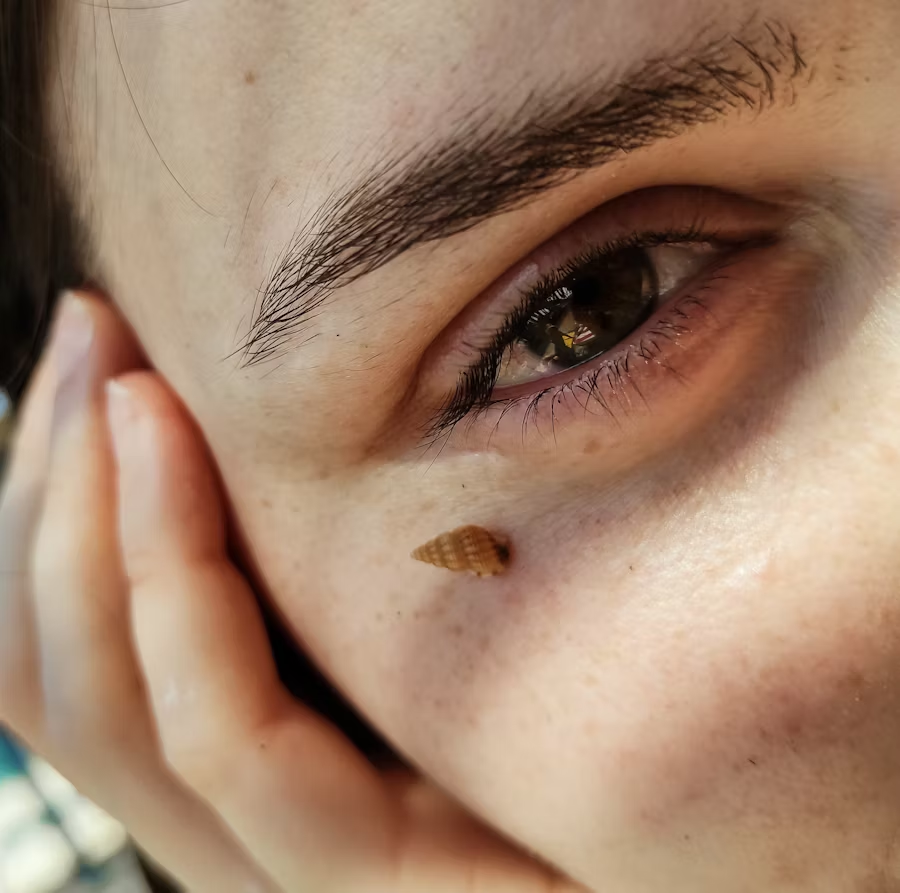
In early flare ups, eczema often appears as:
During chronic or older eczema, skin can become:
These variations can answer the question: “what does eczema look like?” depending on where you are in your flare cycle.
This is the most common form of eczema and often starts in childhood. Here’s how atopic dermatitis looks:
Because atopic dermatitis is often widespread and persistent, early moisturization and skincare, such as using NellaCalm by NellaDerm (steroid-free and fragrance-free), are essential in managing visible symptoms.
Contact dermatitis appears where the skin touches an allergen or irritant:
This type may answer the question, “what does eczema look like when it’s triggered by a product or item?” If you suspect contact dermatitis, avoid the offending irritant and use barrier protection after handwashing.
Nummular is distinctive and easy to spot once you know what to look for:
These coin-shaped spots can bleed or become crusty if scratched, making the presentation more dramatic. Nummular eczema often requires longer-term emollient therapy and topical treatments to resolve.
This type looks different than other eczema forms:
Dyshidrotic eczema can look like tiny bubbles under the skin rather than red patches. Recognizing this type answers the question, “what does eczema look like on hands or feet during flare ups?”
Though technically a separate condition, seborrheic dermatitis can overlap with eczema:
On skin of color, the patches may appear more brown or gray, but the greasy scaling remains noticeable.
When trying to answer “what does eczema look like?” it’s important to acknowledge variation across skin tones:
| Skin Tone | Early Flare | Chronic Phase |
| Light / Fair | Bright red, dry | Pink or brown toughened skin |
| Medium / Olive | Pinkish brown or purple | Brown, hyperpigmented or textured areas |
| Dark / Deep | Ashy gray, deep purple, or dark brown | Darker patches, thickened and less inflamed in appearance |
Eczema in deeper skin tones is often underdiagnosed. While redness may not be obvious, itching, swelling, and scaling are still key clues, and dermatologists should evaluate these signs carefully.
Though visual inspection often suffices, professionals may use:
These steps help distinguish eczema from psoriasis, fungal infections, or other dermatologic conditions, ensuring proper diagnosis and treatment.
Below is a verbal visual tour:
Together, these examples give a practical answer to the question “what does eczema look like?” in real life.
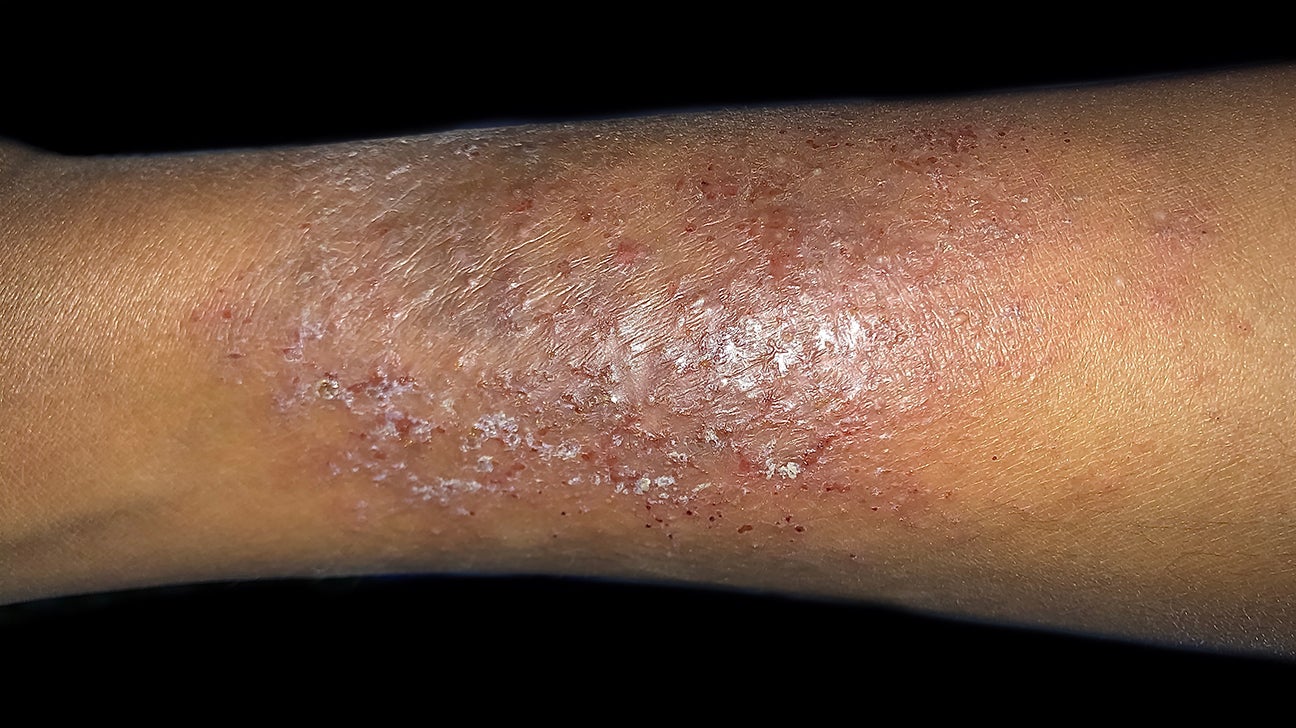
Despite variations in appearance, calming eczema follows a shared skin-first approach:
Consistent hydration helps lessen scaling, thickening, and visible redness over time.
You may also find our related article helpful: How to Wash Bedding for Eczema A Step by Step Guide.
This post highlights common nighttime triggers, such as dust mites, that can influence how eczema looks and feels.
To understand visual patterns and diagnostic criteria, a landmark study in NIH found that eczema severity correlates with skin barrier proteins, redness intensity, and scaling patterns in both children and adults.
If your eczema:
…you should consult a board-certified dermatologist for evaluation. Treatment may include prescription creams, light therapy, or even biologic medications.
When someone asks, “what does eczema look like?”, the answer is: it depends. From red inflamed patches to dark, thickened skin; from tiny blisters on hands to greasy scaling in seborrheic areas, the appearance can be very diverse.
By recognizing these patterns and knowing when to seek care, you can identify eczema early and take steps for relief. Whether your eczema shows as coin-like discs, flaky patches across the scalp, or thickened skin behind joints, the right skincare and professional support can make a difference.
To support daily relief and skin rebuilding, explore gentle, irritation-tested options like NellaDerm’s NellaCalm moisturizer. And for ongoing education, visit the Eczema Knowledge Hub on NellaDerm for visual guides, prevention tips, and product support.
Understanding what causes eczema to progress from early flares to chronic conditions is crucial for effective management. Genetic factors play a significant role, as individuals with a family history of allergies or asthma are more prone to developing atopic dermatitis, the most common type. Environmental triggers such as pollen, dust mites, and pet dander can initiate early inflammation, leading to red patches and itching.
As eczema advances to chronic stages, repeated scratching damages the skin barrier, causing thickening and lichenification. Dry weather, harsh soaps, and stress exacerbate this progression by increasing inflammation and impairing skin repair. Food allergens like dairy or nuts may trigger flares in some people, while others experience worsening from sweat or friction during physical activity.
Infections, particularly bacterial ones like Staphylococcus aureus, can turn acute eczema chronic by colonizing cracked skin. Hormonal changes, such as during puberty or pregnancy, also influence severity. Identifying personal triggers through journaling or allergy testing helps prevent progression, allowing for targeted interventions that keep skin in the early, more manageable stage.
Overall, a combination of genetics, environment, and lifestyle factors drives eczema from initial redness to persistent scaling. Early recognition and avoidance of triggers can slow this evolution, improving long-term skin health.
While visual changes are prominent, eczema’s impact extends to sensations that affect daily life. In early stages, intense itching often precedes visible redness, creating an urge to scratch that can disrupt sleep and concentration. This pruritus feels like a persistent tickle or burn, worsening at night or with heat exposure.
As it becomes chronic, pain joins the itch due to cracked, thickened skin. Sensitivity to touch increases, making clothing or bedding uncomfortable. Emotional symptoms like anxiety or frustration arise from constant discomfort, potentially leading to social withdrawal. Children may experience growth delays or behavioral issues from poor sleep.
Systemic effects include fatigue from immune overactivity and increased allergy risks. In severe cases, secondary infections cause warmth, swelling, or pus. Recognizing these non-visual symptoms alongside appearance changes ensures comprehensive care, addressing both physical and mental aspects of eczema.
Managing these feelings involves anti-itch creams, stress reduction techniques, and professional support. By treating the whole experience, not just the look, individuals can achieve better quality of life across all stages.
Tailoring treatment to eczema’s stage optimizes results and prevents worsening. For early flares, focus on reducing inflammation quickly with topical corticosteroids or calcineurin inhibitors prescribed by a doctor. These calm redness and itching, preventing scratches that lead to infection.
Moisturizers are vital at every stage but especially early, locking in hydration to support the barrier. Natural options with ceramides or oats soothe without steroids. In chronic phases, thicker ointments address lichenification, applied after bathing for better absorption.
Advanced treatments like phototherapy or biologics target persistent cases, reducing immune overactivity. Wet wrap therapy, involving medicated creams under damp bandages, provides intense relief for severe chronic areas. Oral medications may be needed for widespread involvement.
Lifestyle integration includes trigger avoidance and routine skincare. Regular follow-ups with dermatologists adjust plans as stages evolve. This staged approach minimizes symptoms, promoting clearer, more comfortable skin over time.
Remember, what works early may need intensification chronically. Patience and consistency yield the best outcomes in managing this progressive condition.
Preventing eczema from advancing requires proactive measures. Daily moisturizing strengthens the skin barrier, reducing flare likelihood. Choose fragrance-free products and apply liberally, especially after showers when skin is damp.
Environmental controls like using humidifiers in dry climates maintain moisture levels. Gentle laundry detergents without dyes prevent irritation from clothing. Diet adjustments, avoiding known allergens, can limit internal triggers.
Stress management through exercise or mindfulness curbs cortisol-driven flares. Protective gloves during chores shield hands from irritants. For children, early intervention with emollients may prevent chronic development.
Regular check-ups catch changes early. By implementing these habits, many halt progression, keeping eczema in milder stages for improved daily comfort.
Misconceptions about eczema stages can hinder proper care. One myth is that eczema is always red; on darker skin, it appears gray or purple. Another claims it’s contagious, but it’s an immune condition, not infectious.
Some believe outgrowing it happens automatically, yet many adults experience chronic forms. The idea that diet cures all ignores genetic factors. Scratching doesn’t cause it but worsens progression.
Natural remedies aren’t always safe; some irritate further. Understanding facts empowers better management across stages.
Consult reliable sources to separate truth from fiction, ensuring informed decisions for skin health.
Emerging research promises better understanding of eczema stages. Studies on microbiome influences explore how gut bacteria affect progression. Gene therapy targets root causes for long-term remission.
Personalized medicine uses biomarkers to predict chronic risk. New topicals with anti-inflammatory peptides show promise without steroid side effects. Clinical trials for biologics expand options for severe cases.
AI diagnostics improve early detection through image analysis. As knowledge grows, treatments become more effective, potentially altering how we view and manage eczema stages.
Staying updated on advancements offers hope for those navigating this condition.
Q: Can it resemble psoriasis or a fungal rash?
A: Yes—especially in chronic or scaly forms. That’s why accurate diagnosis matters.
Q: Does eczema leave scars or marks?
A: It can cause post-inflammatory pigmentation or thickened patches if untreated or over-scratched.
It’s easy to apply and isn’t chalky at all. I’ve been applying it multiple times a day… I’ve tried multiple new products to try and treat my eye eczema, and this is definitely the best I’ve tried so far.
My 7-year old son has been dealing with eczema on his face for a long time, and it’s been so tough to find something that really works…..I’m amazed by the results! Within one day, the redness and rough patches on his face significantly improved…. he doesn’t mind using it at all because it doesn’t sting or feel greasy. – Lily




Like many of you, our eczema journey is personal. That’s why we’re committed to creating a space for the eczema community to share experiences, be empowered through evidence-based solutions, and learn practical tips for daily life.
– Sajjad, Founder & CEO of NellaDerm
